Abstract
Compared to other races/ethnicities, the Latino population has a lower rate of adherence to colorectal cancer (CRC) screening guidelines. Previous studies have identified a variety of barriers to CRC screening in Latino populations but have not explored factors associated with barriers. The purpose of this study was to identify barriers to CRC screening and associated factors in a Midwest Latino population visiting an urban Federally Qualified Health Center (FQHC). We conducted a cross-sectional investigation of 68 Latinos at a FQHC from June to October 2017. We examined factors associated with scheduling, psychological, and financial barriers using t-test, ANOVA, and multiple linear regression analyses. Our participants reported low educational level, low income, and limited access to insurance or a primary care provider. Scheduling barriers are the highest barrier compared with psychological and financial barriers. Being married or coupled was the only predictor of higher scheduling barriers (P < .05). Being married or coupled was associated with higher psychological barriers in both univariate and multivariate analysis (P < .05). Higher education level was associated with higher psychological barriers in univariate (P < .05) but not multivariate analysis. Participants with lower vs. higher English proficiency had a higher financial barrier score in univariate (P < .05) but not multivariate analysis. Despite interventions targeting CRC screening barriers, including the provision of free at-home testing, perceived barriers persist. Bilingual patient navigators may help address needs for those with limited English proficiency to find and schedule free or reduced-fee colonoscopy services. People who are well educated are also at high risk of psychological barriers and should be targeted and given more education on the importance of CRC screening.
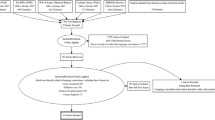
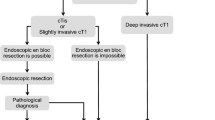
Similar content being viewed by others
Data availability
Not applicable.
Code Availability
Not applicable.
References
U.S. Census Bureau (2019) Quick facts (United States). https://www.census.gov/quickfacts/fact/table/US/PST045219. Accessed 28 June 2020.
Heron M (2019) Deaths: Leading causes for 2017. http://www.cdc.gov/nchs/data/nvsr/nvsr68/nvsr68_06-508.pdf. Accessed 4 April 2021.
American Cancer Society (2018) Cancer Facts & Figures for Hispanics/Latinos 2018-2020. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/cancer-facts-and-figures-for-hispanics-and-latinos/cancer-facts-and-figures-for-hispanics-and-latinos-2018-2020.pdf. Accessed 4 April 2021.
Mandel JS, Bond JH, Church TR et al (1993) Reducing mortality from colorectal cancer by screening for fecal occult blood. N Eng J Med 328(19):1365–1371. https://doi.org/10.1056/NEJM199305133281901
Bibbins-Domingo K, Grossman DC, Curry SJ et al (2016) Screening for colorectal cancer: US preventive services task force recommendation statement. J Am Med Assoc 315(23):2564–2575. https://doi.org/10.1001/jama.2016.5989
Zhu M, Chu H, Greenland S (2011) Biased standard errors from complex survey analysis: an example from applying ordinary least squares to the national hospital ambulatory medical care survey. Ann Epidemiol 21(11):830–834. https://doi.org/10.1016/j.annepidem.2011.08.003
Geiger TM, Ricciardi R (2009) Screening options and recommendations for colorectal cancer. Clin Colon Rectal Surg 22(4):209–217. https://doi.org/10.1055/s-0029-1242460
Joseph DA, King JB, Dowling NF, Thomas CC, Richardson LC (2020) Vital signs: colorectal cancer screening test use—United States, 2018. Morb Mortal Wkly Rep 69(10):253. https://doi.org/10.15585/mmwr.mm6910a1
Centers for Disease Control and Prevention (2017) 2016 Behavioral Risk Factor Surveillance System Questionnaire. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. https://www.cdc.gov/brfss/annual_data/annual_2016.html. Accessed 17 May 2020.
National Cancer Institute (2021) State Cancer Profiles – Nebraska. https://statecancerprofiles.cancer.gov/quick-profiles/index.php?statename=nebraska#t=1. Accessed 6 May 2021.
Zhu M, Chu H, Rice TM, Carter MW (2011) Implications of conducting trend analyses of emergency department visits using publicly released masked design variables. Ann Emerg Med 57(6):683-687.e681. https://doi.org/10.1016/j.annemergmed.2010.12.025
Fernandez ME, Wippold R, Torres-Vigil I et al (2008) Colorectal cancer screening among Latinos from U.S. cities along the Texas-Mexico border. Cancer Causes Control 19(2):195–206. https://doi.org/10.1007/s10552-007-9085-6
Coronado GD, Petrik AF, Spofford M, Talbot J, Do HH, Taylor VM (2015) Clinical perspectives on colorectal cancer screening at Latino-serving federally qualified health centers. Health Educ Behav 42(1):26–31. https://doi.org/10.1177/1090198114537061
Warner EL, Bodson J, Mooney R, Lai D, Samadder NJ, Kepka D (2018) Latinas’ colorectal cancer screening knowledge, barriers to receipt, and feasibility of home-based fecal immunochemical testing. J Immigr Minor Health 20(4):981–990. https://doi.org/10.1007/s10903-017-0615-3
Byrd TL, Calderón-Mora J, Salaiz R, Shokar NK (2019) Barriers and facilitators to colorectal cancer screening within a Hispanic population. Hisp Health Care Int 17(1):23–29. https://doi.org/10.1177/1540415318818982
Valdovinos C, Penedo FJ, Isasi CR et al (2016) Perceived discrimination and cancer screening behaviors in US Hispanics: the Hispanic Community Health Study/Study of Latinos Sociocultural Ancillary Study. Cancer Causes Control 27(1):27–37. https://doi.org/10.1007/s10552-015-0679-0
Mojica CM, Parra-Medina D, Vernon S (2018) Interventions promoting colorectal cancer screening among Latino men: a systematic review. Prev Chronic Dis 15:E31. https://doi.org/10.5888/pcd15.170218
Health R, Services A. 2017. 2017 One World Community Health Centers Health Center Profile. HRSA Health Center Program.
Hesse BW, Greenberg AJ, Peterson EB, Chou WS (2017) The Health Information National Trends Survey (HINTS): a resource for consumer engagement and health communication research. Stud Health Technol Inform 240:330–346
Cantor D, Covell J, Davis T, Park I, Rizzo L (2005) Health information national trends survey 2005 (HINTS 2005): Final Report. https://hints.cancer.gov/docs/HINTS_2005_Final_Report.pdf. Accessed 4 April 2021.
Green AR, Peters-Lewis A, Percac-Lima S et al (2008) Barriers to screening colonoscopy for low-income Latino and white patients in an urban community health center. J Gen Int Med 23(6):834–840. https://doi.org/10.1007/s11606-008-0572-6
Giorgi Rossi P, Grazzini G, Anti M et al (2011) Direct mailing of faecal occult blood tests for colorectal cancer screening: a randomized population study from Central Italy. J Med Screen 18(3):121–127. https://doi.org/10.1258/jms.2011.011009
Community Preventive Services Task Force (2010) Cancer screening: reducing structural barriers for clients –colorectal cancer. https://www.thecommunityguide.org/findings/cancer-screening-reducing-structural-barriers-clients-colorectal-cancer. Accessed 4 April 2021.
Nebraska Colon Cancer Screening Program (2020) Lincoln: Nebraska Department of Health and Human Services. http://dhhs.ne.gov/Pages/Nebraska-Colon-Cancer-Screening-Program.aspx. Accessed 28 July 2020.
Hopemed.us (2019) Omaha: Hope Medical Outreach Coalition. http://hopemed.us/. Accessed 28 July 2020.
Programs & Services - Access to Care (2017) Lincoln: Lancaster County Medical Society. http://www.lcmsne.org/access-to-care.html. Accessed 28 July 2020.
Acknowledgements
We would like to thank Dr. Kristine McVea for helpful discussions regarding this work, Roger Gonzales for help with data collection, and Dr. Armando De Alba for help with questionnaire translation.
Funding
The work was supported by a University of Nebraska Medical Center College of Public Health Innovation grant and funding from the Nebraska Research Initiative.
Author information
Authors and Affiliations
Contributions
K.R.: data analysis and manuscript writing; K.C.: data analysis and manuscript writing; S.W.G.: data analysis and manuscript writing; P.A.F.: study conceptualization and design, data analysis, manuscript writing, and overall overseeing of the study
Corresponding author
Ethics declarations
Ethics Approval
The study protocol was reviewed by the University of Nebraska Medical Center Institutional Review Board prior to data collection and deemed exempt.
Consent to Participate
The interviewer described the study and obtained verbal informed consent from those who agreed to participate to keep responses anonymous.
Consent for Publication
All authors approved the final manuscript and agreed with submission and publication.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ratnapradipa, K.L., Chen, K., Watanabe-Galloway, S. et al. Cross-sectional Study of Colorectal Cancer Screening Barriers in a Latino-Serving Federally Qualified Health Center. J Canc Educ 38, 193–200 (2023). https://doi.org/10.1007/s13187-021-02097-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-021-02097-w