Abstract
Background
Racial concordance between patients and clinician has been linked to improved satisfaction and patient outcomes.
Objectives
(1) To examine the likelihood of clinician-patient racial concordance in non-Hispanic White, non-Hispanic Black, Asian, and Hispanic patients and (2) to evaluate the impact of patient-clinician race concordance on healthcare use and expenditures within each racial ethnic group.
Methods
We analyzed data from the 2010–2016 Medical Expenditure Panel Survey (MEPS). We used bivariate and multivariate models to assess the association between patient-clinician race concordance and emergency department (ED) use, hospitalizations, and total healthcare expenses, controlling for patient socio-demographic factors, insurance coverage, health status, and survey year fixed effects.
Results
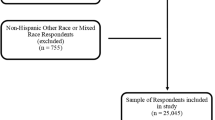
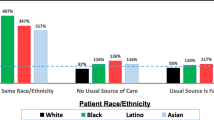
Of the 50,626 adults in the analysis sample, 32,350 had racial concordance with their clinician. Among Asian and Hispanic patients, low income, less education, and non-private insurance were associated with an increased likelihood of patient-clinician racial concordance. Emergency department use was lower among Whites and Hispanics with concordant clinicians compared to those without a discordant clinician (15.6% vs. 17.3%, p = 0.02 and 12.9% vs. 16.2%, p = 0.01 respectively). Total healthcare expenditures were lower among Black, Asian, and Hispanic patients with race-concordant clinicians than those with discordant clinicians (14%, 34%, and 20%, p < 0.001 respectively).
Conclusions
These results add to the body of evidence supporting the hypothesis that racial concordance contributes to a more effective therapeutic relationship and improved healthcare. These results emphasize the need for medical education surrounding cultural humility and the importance of diversifying the healthcare workforce.



Similar content being viewed by others
Change history
24 February 2021
A Correction to this paper has been published: https://doi.org/10.1007/s40615-021-01003-w
References
Braveman P. Health disparities and health equity: concepts and measurement. Annu Rev Public Health. 2006;27(1):167–94. https://doi.org/10.1146/annurev.publhealth.27.021405.102103.
2016 National Healthcare Quality and Disparities Report. Rockville, MD: Agency for Healthcare Research and Quality; 2017.
Penner LA, Hagiwara N, Eggly S, Gaertner SL, Albrecht TL, Dovidio JF. Racial healthcare disparities: a social psychological analysis. Eur Rev Soc Psychol. 2013;24(1):70–122. https://doi.org/10.1080/10463283.2013.840973.
Saha S, Arbelaez JJ, Cooper LA. Patient–physician relationships and racial disparities in the quality of health care. Am J Public Health. 2003;93(10):1713–9. https://doi.org/10.2105/AJPH.93.10.1713.
Kirby JB, Taliaferro G, Zuvekas SH. Explaining racial and ethnic disparities in health care: Med Care. 2006;44(suppl):I-64-I-72. https://doi.org/10.1097/01.mlr.0000208195.83749.c3
Elster A, Jarosik J, VanGeest J, Fleming M. Racial and ethnic disparities in health care for adolescents: a systematic review of the literature. Arch Pediatr Adolesc Med. 2003;157(9):867–74. https://doi.org/10.1001/archpedi.157.9.867.
McGuire TG, Alegria M, Cook BL, et al. Implementing the Institute of Medicine definition of disparities: an application to mental health care. Health Serv Res. 2006;41(5):1979–2005. https://doi.org/10.1111/j.1475-6773.2006.00583.x.
Fernandez A, Schillinger D, Warton EM, Adler N, Moffet HH, Schenker Y, et al. Language barriers, physician-patient language concordance, and glycemic control among insured Latinos with diabetes: the diabetes study of Northern California (DISTANCE). J Gen Intern Med. 2011;26(2):170–6. https://doi.org/10.1007/s11606-010-1507-6.
Parker MM, Fernández A, Moffet HH, Grant RW, Torreblanca A, Karter AJ. Association of patient-physician language concordance and glycemic control for limited–English proficiency Latinos with type 2 diabetes. JAMA Intern Med. 2017;177(3):380–7. https://doi.org/10.1001/jamainternmed.2016.8648.
Paasche-Orlow MK, Parker RM, Gazmararian JA, Nielsen-Bohlman LT, Rudd RR. The prevalence of limited health literacy. J Gen Intern Med. 2005;20(2):175–84. https://doi.org/10.1111/j.1525-1497.2005.40245.x.
Osborn CY, Paasche-Orlow MK, Davis TC, Wolf MS. Health literacy. Am J Prev Med. 2007;33(5):374–8. https://doi.org/10.1016/j.amepre.2007.07.022.
Unequal treatment: confronting racial and ethnic disparities in health care (with CD). Washington, D.C.: National Academies Press; 2003. https://doi.org/10.17226/12875
De Lew N, Weinick R. An overview: eliminating racial, ethnic, and SES disparities in health care. Health Care Financ Rev. 2000;21(4):7.
Shen MJ, Peterson EB, Costas-Muñiz R, Hernandez MH, Jewell ST, Matsoukas K, et al. The effects of race and racial concordance on patient-physician communication: a systematic review of the literature. J Racial Ethn Health Disparities. 2018;5(1):117–40. https://doi.org/10.1007/s40615-017-0350-4.
Hernandez ND, Daley EM, Young L, Kolar SK, Wheldon C, Vamos CA, et al. HPV vaccine recommendations: does a health care clinician’s gender and ethnicity matter to unvaccinated Latina college women? Ethn Health. 2019;24(6):645–61. https://doi.org/10.1080/13557858.2017.1367761.
Saha S, Taggart SH, Komaromy M, Bindman AB. Do patients choose physicians of their own race? To provide the kind of care consumers want, medical schools might be able to justify using race as an admissions criterion. Health Aff (Millwood). 2000;19(4):76–83. https://doi.org/10.1377/hlthaff.19.4.76.
Brown TT, Scheffler RM, Tom SE, Schulman KA. Does the market value racial and ethnic concordance in physician? patient relationships? Health Serv Res. 2007;42(2):706–26. https://doi.org/10.1111/j.1475-6773.2006.00634.x.
Cooper LA, Roter DL, Johnson RL, Ford DE, Steinwachs DM, Powe NR. Patient-centered communication, ratings of care, and concordance of patient and physician race. Ann Intern Med. 2003;139(11):907–15. https://doi.org/10.7326/0003-4819-139-11-200312020-00009.
Penner LA, Gaertner S, Dovidio JF, Hagiwara N, Porcerelli J, Markova T, et al. A social psychological approach to improving the outcomes of racially discordant medical interactions. J Gen Intern Med. 2013;28(9):1143–9. https://doi.org/10.1007/s11606-013-2339-y.
Persky S, Kaphingst KA, Allen VC, Senay I. Effects of patient-clinician race concordance and smoking status on lung cancer risk perception accuracy among African-Americans. Ann Behav Med. 2013;45(3):308–17. https://doi.org/10.1007/s12160-013-9475-9.
Metzl JM, Roberts DE. Structural competency meets structural racism: race, politics, and the structure of medical knowledge. AMA J Ethics. 2014 Sep 1;16(9):674–90.
Tervalon M. and Murray-García, J. Cultural humility versus cultural competence: a critical distinction in defining physician training outcomes in multicultural education. Journal of Healthcare for the Poor and Underserved. May 1998. .
Street RL, O’Malley KJ, Cooper LA, et al. Understanding concordance in patient-physician relationships: personal and ethnic dimensions of shared identity. Ann Fam Med. 2008;6(3):198–205. https://doi.org/10.1370/afm.821.
Laveist TA, Nuru-Jeter A. Is doctor-patient race concordance associated with greater satisfaction with care? J Health Soc Behav. 2002;43(3):296–306.
Cooper-Patrick L. Race, gender, and partnership in the patient-physician relationship. JAMA. 1999;282(6):583–9. https://doi.org/10.1001/jama.282.6.583.
Alsan M, Garrick O, Graziani G. Does diversity matter for health? Experimental evidence from Oakland. :60.
Greenwood BN, Hardeman RR, Huang L, Sojourner A. Physician–patient racial concordance and disparities in birthing mortality for newborns. Proc Natl Acad Sci. 2020 Aug;13.
Oguz T. Is patient-provider racial concordance associated with Hispanics’ satisfaction with health care? Int J Environ Res Public Health. 2019 Jan;16(1):31.
Nimbal VC, Zhao B, Pu J, Romanelli RJ, Palaniappan L, Chung S. Does patient-provider racial/ethnic and language concordance impact patient-reported experience of care? J Patient Cent Res Rev. 2016;3:198.
Han W, Lee S. Racial/ethnic variation in health care satisfaction: the role of acculturation. Soc Work Health Care. 2016 Oct 20;55(9):694–710.
Kumar D, Schlundt DG, Wallston KA. Patient-physician race concordance and its relationship to perceived health outcomes. Ethnicity & Disease. 2009;19(3):345–51.
Lasser K. Missed appointment rates in primary care: the importance of site of care. J Health Care Poor Underserved. 2005;16(3):475–86. https://doi.org/10.1353/hpu.2005.0054.
Xierali IM, Nivet MA. The racial and ethnic composition and distribution of primary care physicians. J Health Care Poor Underserved. 2018;29(1):556–70. https://doi.org/10.1353/hpu.2018.0036.
Traylor AH, Schmittdiel JA, Uratsu CS, Mangione CM, Subramanian U. Adherence to cardiovascular disease medications: does patient-clinician race/ethnicity and language concordance matter? J Gen Intern Med. 2010;25(11):1172–7. https://doi.org/10.1007/s11606-010-1424-8.
King WD, Wong MD, Shapiro MF, et al. Does racial concordance between HIV-positive patients and their physicians affect the time to receipt of protease inhibitors? 2004;19:9.
Saha S, Komaromy M, Koepsell TD, Bindman AB. Patient-physician racial concordance and the perceived quality and use of health care. Arch Intern Med. 1999;159(9):997–1004. https://doi.org/10.1001/archinte.159.9.997.
Strumpf EC. Racial/ethnic disparities in primary care: the role of physician-patient concordance. Med Care. 2011;49(5):496–503. https://doi.org/10.1097/MLR.0b013e31820fbee4.
Hagiwara N, Slatcher RB, Eggly S, Penner LA. Physician racial bias and word use during racially discordant medical interactions. Health Commun. 2017;32(4):401–8. https://doi.org/10.1080/10410236.2016.1138389.
Meghani SH, Brooks JM, Gipson-Jones T, Waite R, Whitfield-Harris L, Deatrick JA. Patient–clinician race-concordance: does it matter in improving minority patients’ health outcomes? Ethn Health. 2009;14(1):107–30. https://doi.org/10.1080/13557850802227031.
Bazemore A, Petterson S, Peterson LE, Bruno R, Chung Y, Phillips RL. Higher primary care physician continuity is associated with lower costs and hospitalizations. The Annals of Family Medicine. 2018 Nov 1;16(6):492–7.
Bazemore A, Petterson S, Peterson LE, Phillips RL. More comprehensive care among family physicians is associated with lower costs and fewer hospitalizations. The Annals of Family Medicine. 2015 May 1;13(3):206–13.
Ma A, Sanchez A, Ma M. The impact of patient-provider race/ethnicity concordance on provider visits: updated evidence from the Medical Expenditure Panel Survey. J Racial Ethn Health Disparities. 2019 Oct 1;6(5):1011–20.
Chowdhury S, Machlin S, Gwet K. Sample designs of the Medical Expenditure Panel Survey Household Component, 1996–2006 and 2007–2016. Rockville, MD: Agency for Healthcare Research and Quality; 2019. https://meps.ahrq.gov/data_files/publications/mr33/mr33.pdf
Medical Expenditure Panel Survey. Agency for Healthcare Research and Quality https://meps.ahrq.gov/mepsweb/datastats/downloaddatafiles.jsp%20Accessed%20February%202019
StataCorp. Stata Statistical Software. College Station, Tx: StataCorp LP; 2015.
Liaw W, Petterson S, Rabin DL, Bazemore A. The impact of insurance and a usual source of care on emergency department use in the United States. International journal of family medicine. 2014;2014:1–5.
The United States Census Bureau. Comparative Demographic Estimates 2016 American Community Survey 1-Year Estimates. https://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=ACS_16_1YR_CP05&prodType=table. .
Villani J, Mortensen K. Nonemergent emergency department use among patients with a usual source of care.
Malhotra J, Rotter D, Tsui J, Llanos AA, Balasubramanian BA, Demissie K. Impact of patient–provider race, ethnicity, and gender concordance on cancer screening: findings from Medical Expenditure Panel Survey. Cancer Epidemiology and Prevention Biomarkers. 2017 Dec 1;26(12):1804–11.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jetty, A., Jabbarpour, Y., Pollack, J. et al. Patient-Physician Racial Concordance Associated with Improved Healthcare Use and Lower Healthcare Expenditures in Minority Populations. J. Racial and Ethnic Health Disparities 9, 68–81 (2022). https://doi.org/10.1007/s40615-020-00930-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-020-00930-4