Abstract
Objective
To determine if a self-administered previsit questionnaire designed to increase awareness of patients’ concerns alters the visit duration, content of the discussion, and patient and physician satisfaction.
Design
A balanced, two-arm trial in which physicians were randomized.
Setting
Two primary-care clinics affiliated, with a university hospital.
Patients/Participants
Ten physicians and 201 continuitycare patients.
Interventions
In intervention visits, patients completed a previsit questionnaire asking about the desire for medical information, psychosocial assistance, therapeutic listening, general health advice, and biomedical treatment. Physicians reviewed questionnaires with patients during the visit.
Measurements and main results
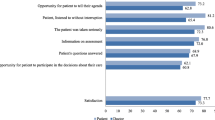
We used audiotapes of encounters to quantify the duration of the encounter and measured the number and type of diagnoses discussed in the visit, and patient and physician satisfaction with the encounter. Intervention visits were 34% longer (increase of 6.8 minutes; 95% confidence interval, [CI] 0.4, 13.2) than control visits with most of the additional time spent in discussion of biomedical diagnoses (3.35 minutes; 95% CI 0.00, 6.72) and in the performance of the physical examination (2.7 minutes; 95% CI 0.5 4.9). The number of diagnoses discussed per visit was 30% higher in intervention visits (increase of 1.7 diagnoses per visit; 95% CI 0.3, 3.2), but patients’ satisfaction with these visits tended to be lower.
Conclusions
Using a previsit questionnaire to increase awareness of the patients’ concerns may entail a trade-off between conflicting goals: trying to respond to patient concerns while not significantly increasing the cost per visit. A future challenge is to develop and refine techniques with sufficient efficacy to justify the expense of implementing the intervention and the longer visit needed to respond adequately to patients’ concerns.
Similar content being viewed by others
References
Roland MO, Bartholomew J, Courtnenay MJF, Morris RW, Morrell DC. The “five minute” consultation: effect of time constraint on verbal communication. BMJ. 1986;292:874–5.
Franks P, Nutting PA. Health care reform, primary care, and the need for research. JAMA. 1993;270:1449–53.
Alper PR, Primary care in transition, JAMA. 1994;272(19):1523–7.
Scheingold L. Office efficiency in primary care. HMO Pract. 1990. 4:66–70.
Camasso MJ, Camasso AE. Practitioner productivity and the product content of medical care in publicly supported health centers. Soc Sci. Med. 1994;38:733–48.
Mason JL, Barkley SE, Kappelman MM, Carter DE, Beachy WV. Evaluation of a self-instructional method for improving doctor-patient communication. J Med Educ. 1988;63:629–35.
Johnson A, Adelstein DJ. The use of recorded interviews to enhance physician-patient communication. Cancer Educ. 1991;6(2): 99–102.
Levinson W, Roter D. The effects of two continuing medical education programs on communication skills of practicing primary care physicians. J Gen Intern Med. 1993;8(6):318–24.
Joos SK, Hickman DH, Gordon GH, Baker LH. Effects of a physician communication intervention on patient care outcomes. J Gen Intern Med. 1996;11(3):147–55.
Morgan ER, Winter RJ. Teaching communication skills. An essential part of residency training. Arch Pediatr Adolesc Med. 1996; 150(6):638–42.
Roter DL. Patient participation in the patient-provider interaction: the effects of patient question asking on the quality of interaction satisfaction and compliance. Health Educ Monogr. 1977;5(4):281–315.
Žimney L, McClain MP, Batalden PB, O’Connor JP. Patient telephone interviews: a valuable technique for finding problems and assessing quality in ambulatory medical care. J Community Health. 1980;6(1):35–42.
Greenfield S, Kaplan S, Ware JE. Expanding patient involvement in care: effect on patient outcomes. Ann Intern Med. 1985;102:520–8.
Anderson LA, DeVellis BM, DeVellis RF. Effects of modeling on patient communication, satisfaction, and knowledge. Med Care. 1987;25(11):1044–56.
Lewis, CC, Pantell RH, Sharp L. Increasing patient knowledge, satisfaction, and involvement: randomized trial of a communication intervention. Pediatrics. 1991;88(2):351–8.
Greenfield S, Kaplan SH, Ware JE, Martin E, Frank HJL. Patients’ participation in medical care: effects on blood sugar control and quality of life in diabetes. J Gen Intern Med. 1988;3:448–57.
Kaplan SH, Greenfield S, Ware JE. Assessing the effects of physician-patient interactions on the outcomes of chronic disease. Med Care. 1989;27(3):S110–27.
Brodman K, Erdmann AJ, Lorge I, Wolff HG, Broadbent TH. The Cornell Medical Index. JAMA. June 11, 1949: 530–4.
Mellner, C. Self-administered medical history: theoretical possibilities and practical limitations of the usefulness of standardized medical histories. Acta Chir Scand. 1970;406 (suppl):4–104.
Lazare A, Eisenthal S. Patient requests in a walk-in clinic. J Nerv Ment Dis. 1977;165(5):330–40.
Inui TS, Jared RA, Carter WB, et al. Effects of a self-aministered health history on new-patient, visits in a general medical clinic. Med Care. 1979;26(12):1221–8.
Good MD, Good BJ, Nassi AJ. Patient requests in primary health care settings: development and validation of a research instrument. J Behav Med. 1983;6(2):151–67.
Like R, Žyzanski SJ. Patient requests in family practice: a focal point for clinical negotiation. Fam Pract 1986;3:216–28.
Nelson EC, Larson CO, Davies AR, Gustafson D, Ferreira PL, Ware JE. The patient comment card: a system to gather customer feedback. Qual Rev Bull. 1991;17:278–86.
Joos SK, Hickam DH, Borders LM. Patient desires and satisfaction in general medicine clinics. Public Health Rep. 1993;108(6):751–9.
Adler LM, Ware JE, Enelow AJ. Changes in medical interviewing style after instruction with two closed-circuit television techniques. J Med Educ. 1970;45(1):21–8.
Burgoyne RW, Staples FR, Yamamoto J, Wolkon GH, Kline F. Patient’s requests of an outpatient clinic. Arch Gen Psychiatry. 1979;36:400–3.
Barsky AJ, Kazis LE, Freiden RB, Goroll AH, Hatem CJ, Lawrence RS. Evaluating the interview in primary care medicine. Soc Sci. Med. 1980;14A:653–8.
Freidin RB, Goldman L, Cecil RR. Patient-physician concordance in problem identification in the primary care setting. Ann Intern Med. 1980;93:490–3.
Eisenthal S, Koopman C, Lazare A. Process analysis of two dimensions of the negotiated approach in relation to satisfaction in the initial interview. J Nerv Ment Dis. 1983;171(1):49–54.
Southgate LJ, Bass MJ. Determination of worries and expectations of family practice patients. J Fam Pract. 1983;16(2):339–44.
Like R, Žyzanski SJ. Patient satisfaction with the clinical encounter: social psychological determinants. Soc Scii Med. 1987;4:351–7.
Kendall M, Stuart A. Distribution Theory. The Advanced Theory of Statistics. 2nd ed, New York, NY: Hafner Publishing: 1963: Vol I.
Ware JE, Sherbourne CD. The MOS 36-item short-form survey (SF-36). I: conceptual framework and item selection. Med Care. 1992;30:473–83.
Žigmond AS, Snaith RP. The hospital, anxiety and depression scale. Acta Psychiatr Scand. 1982;67:361–70.
Ware JE, Snyder MK. Dimensions of patient attitude regarding doctors and medical care services. Med Care. 1975;13:669–82.
Snaith RP, Taylor CM. Rating scales for depression and anxiety: a current perspective. Br J Clin Pharmacol. 1985;19(Suppl 1):17–20S.
Aylard PR, Gooding JH, McKenna PJ, Snaith RP. A validation study of three anxiety and depression self-assessment scales. J Psychosom Res. 1987;31(2):261–8.
Hicks JA, Jenkins JG. The measurement of preoperative anxiety. J R Soc Med. 1988;81(9):517–9.
Wilkinson MJ, Barczak P. Psychiatric screening in general practice: comparison of the general health questionnaire and the hospital anxiety depression scale. J R Coll Gen Pract. 1988;38(312):311–3.
Stewart AL, Greenfield S, Hays RD, et al. Functional status and well-being of patients with chronic conditions: results from the Medical Outcomes Study. JAMA. 1989;262:907–12.
Feightner JW, Worrall G. Early detection of depression by primary care physicians. Can Med Assoc J. 1990;142(11):1215–20.
Stewart AL, Ware JE. Measuring Functioning and Well-Being. The Medical Outcomes Study Approach. Durham, NC: Duke University Press; 1992.
ICPC Working Party; Lamberts H, Wood M, eds. International Classification of Primary Care. Oxford, U.K.: Oxford University Press; 1989.
Bales RF. Interaction Process Analysis. Cambridge, Mass: Addison Wesley Press; 1950.
Wasserman RC, Inui TS. Systematic analysis of clinician-patient interactions: a critique of recent approaches with suggestions for future research. Med Care. 1983;21(3):279–93.
Roter D. Patient question asking in physician-patient interaction. Health Psychol. 1984;3:395–409.
Frankel M. Sampling theory. In: Rossi PH, Wright JD, Anderson AB, eds. Handbook of Survey Research. San Diego, Calif: Academic Press: 1983:35–7.
Good BJ, Good MD. The meaning of symptoms: a cultural hermanentic model for clinical practice. In: Eisenberg L, Kleinman A, eds. The Relevance of Social Science for Medicine. Dordrecht, Netherlands: D. Reidel; 1980.
Roter DL, Hall JA, Katz NR. Patient-physician communication: a descriptive summary of the literature. Patient Educ Counsel. 1988;12:99–119.
Stiles WB. Evaluating medical interview process components. Med Care. 1989;27(2):212–20.
Kravitz RL, Callahan EJ, Paterniti D, Antonius D, Dunham M, Lewis CE. Prevalence and sources of patients’ unmet expectations for care. Ann Intern Med. 1996;125:730–7.
Rost P, Frankel A. The introduction of the older patient’s problems in the medical visit. J Aging Health. 1993;5(3):387–401.
Huber PJ. Robust Statistics. New York, NY: Wiley & Sons; 1981.
Katon W, Sullivan MD. Depression and chronic mental illness. J Clin Psychiatry. 1990;56:3–11.
Roter DL, Hall JA. Studies of doctor-patient interaction. Annu Rev Public Health. 1989;10:163–80.
Jencks SF. Recognition of mental distress and diagnosis of mental disorder in primary care. JAMA. 1985;253(13):1903–7.
Schurman RA, Kramer PD, Mitchell JB. The hidden mental health network: treatment of mental illness by nonpsychiatrist physicians. Arch Gen Psychiatry. 1985;42:89–94.
Schulberg HCL. Mental disorders in the primary care setting: research priorities for the 1990s. Gen Hosp Psychiatry. 1991;13:156–64.
Robbins JM, Kirmayer LJ, Cathebras P, Yaffe MJ, Dworkind M. Physician characteristics and the recognition of depression and anxiety in primary care. Med Care. 1994;32(8):795–812.
Schulberg HC, McClelland M. A conceptual model for educating primary care providers in the diagnosis and treatment of depression. Gen Hosp Psychiatry. 1987;9(1):1–10.
Eisenberg L. Treating depression and anxiety in the primary care setting: closing the gap between knowledge and practice. N Engl J Med. 1992;326:1080–4.
Author information
Authors and Affiliations
Additional information
Dr. Hornberger and Dr. Thom are Picker/Commonwealth Scholars. This study was supported by the Picker Institute, the Association for Health Services Research, and the Good Samaritan Foundation.
Rights and permissions
About this article
Cite this article
Hornberger, J., Thom, D. & MaCurdy, T. Effects of a self-administered previsit questionnaire to enhance awareness of patient’s concerns in primary care. J GEN INTERN MED 12, 597–606 (1997). https://doi.org/10.1046/j.1525-1497.1997.07119.x
Issue Date:
DOI: https://doi.org/10.1046/j.1525-1497.1997.07119.x